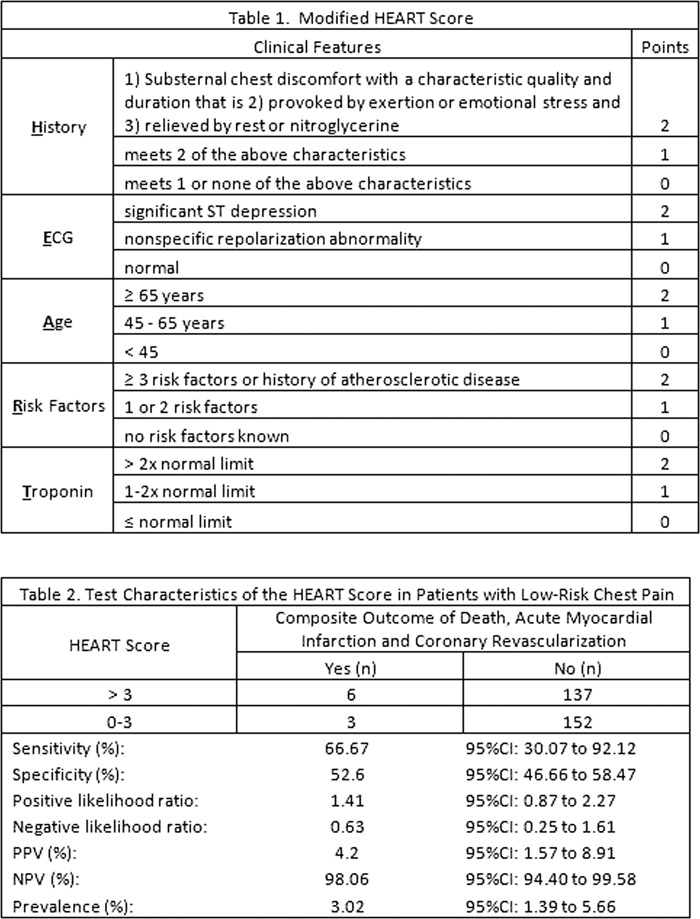 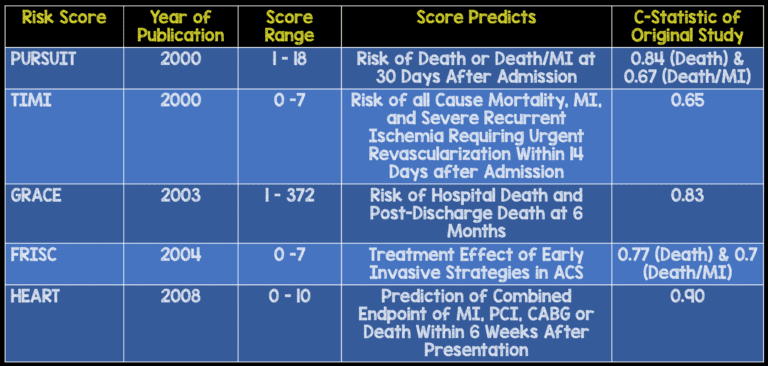
We sought to expand the clinical application of the TIMI risk score by assessing its prognostic accuracy in patients in the emergency department with potential acute coronary syndromes. It was originally developed for use in patients with unstable angina or non–ST-elevation myocardial infarction. Patients with a TIMI risk score of 0 to 2 should be managed medically.Background: The Thrombolysis in Myocardial Infarction (TIMI) risk score uses clinical data to predict the short-term risk of acute myocardial infarction, coronary revascularization or death from any cause. In conclusion, early invasive management, such as cardiac angiography and revascularization, is recommended for patients presenting with a TIMI risk score greater than or equal to 3. Glycoprotein IIb/IIIa inhibitors were shown to decrease the level of myocardial injury, as measured by peak troponin and creatinine kinase levels. The study showed a significant benefit of the use of glycoprotein IIb/IIIa inhibitors with aspirin and heparin in patients with a TIMI score of greater than 4 compared to management with aspirin and heparin alone. The PRISM-PLUS study sought to highlight the importance of glycoprotein IIb/IIIa inhibitors. However, high-risk patients treated with enoxaparin had a significantly reduced risk of major cardiac events on discharge compared to patients treated with unfractionated heparin. Patients who were stratified as high risk had a greater likelihood of presenting with adverse cardiac events. Further studies have taken data from these trials and have shown that nearly a quarter of adverse cardiac events occur within 6 weeks following discharge. The TIMI 11b and ESSENCE trials have shown that nearly one-third of myocardial infarctions and half the number of deaths occur after the first week of presentation. The timing at which certain complications enfold has been another factor of interest. There was no significant difference in outcome between low-risk patients who received early intervention and those who received medical management. After risk stratifying patients, they found that intermediate or high-risk patients who underwent invasive cardiac intervention showed a significant decrease in death, nonfatal MI, and rehospitalization for cardiac events compared to those who were medically managed. The TACTICS-TIMI 18 trial compared outcomes of patients presenting with UA/NSTEMI who underwent either early invasive interventions or conservative treatment with medication. Perhaps the greatest utility that the TIMI score has to offer is its ability to guide the management of patients presenting with signs of unstable angina/non-ST elevated myocardial infarctions (UA/NSTEMI). Nursing, Allied Health, and Interprofessional Team Interventions Recent studies have also shown that the amplitude of ST-segment elevation or depression and the degree of cardiac biomarker elevation (troponin T/I) can both be independent factors that could point toward initiating early invasive cardiac procedures. Studies have also noted that of the seven factors that contribute to the TIMI risk score, history of coronary artery disease, age greater than or equal to 65, and deviations in ST-segment on initial EKG’s were more strongly associated with adverse cardiac events as compared to the other factors. The study found that patients who had a risk score of 5 to 7 were significantly more likely to have severe culprit stenosis, multivessel disease, left main coronary artery disease, or visible thrombus compared to those who were in the low-risk score category. The TIMI risk score was found to be predictive of the severity of the vascular disease, making it a powerful tool to predict the potential blood vessels of coronary circulation that could be involved.Ī sub-study of PRISM-PLUS compared TIMI risk scores to findings on coronary angiography.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
